For many, it is the simplest next step when loud snoring, choking at night, or heavy daytime tiredness starts to feel “normal”.
What is a home sleep study, and what does it test for?
A home sleep study Sydney is an overnight test done in someone’s own bed using a small, portable monitoring device. It is mainly used to assess breathing-related sleep disorders, especially obstructive sleep apnoea (OSA).
Most home studies track airflow, oxygen levels, breathing effort, heart rate, and body position. The results help clinicians estimate how often breathing reduces or stops during sleep and whether oxygen drops into an unsafe range.
Who in Sydney should consider a home sleep study?
They should consider it if symptoms suggest sleep apnoea or another breathing-related sleep disorder. Common triggers include loud snoring, witnessed pauses in breathing, gasping, morning headaches, and persistent daytime sleepiness.
It is also commonly considered for people with high blood pressure, type 2 diabetes, atrial fibrillation, or weight gain where sleep apnoea could be contributing. If their job involves driving, machinery, or safety-critical work, testing can be particularly important.
How fast can they get tested and receive results?
Many providers in Sydney can organise home sleep testing within days, sometimes even same week, depending on referrals and device availability. Because it avoids lab scheduling, it is often quicker than an in-clinic study.
Results time varies by clinic workflow. Some services provide a report within a few business days after the device is returned, while others may take longer if a specialist review and appointment are needed.
What happens during the test at home?
They are typically shown how to apply the sensors or given written and video instructions. The setup is designed to be simple; then they sleep as normally as possible while the device records data.
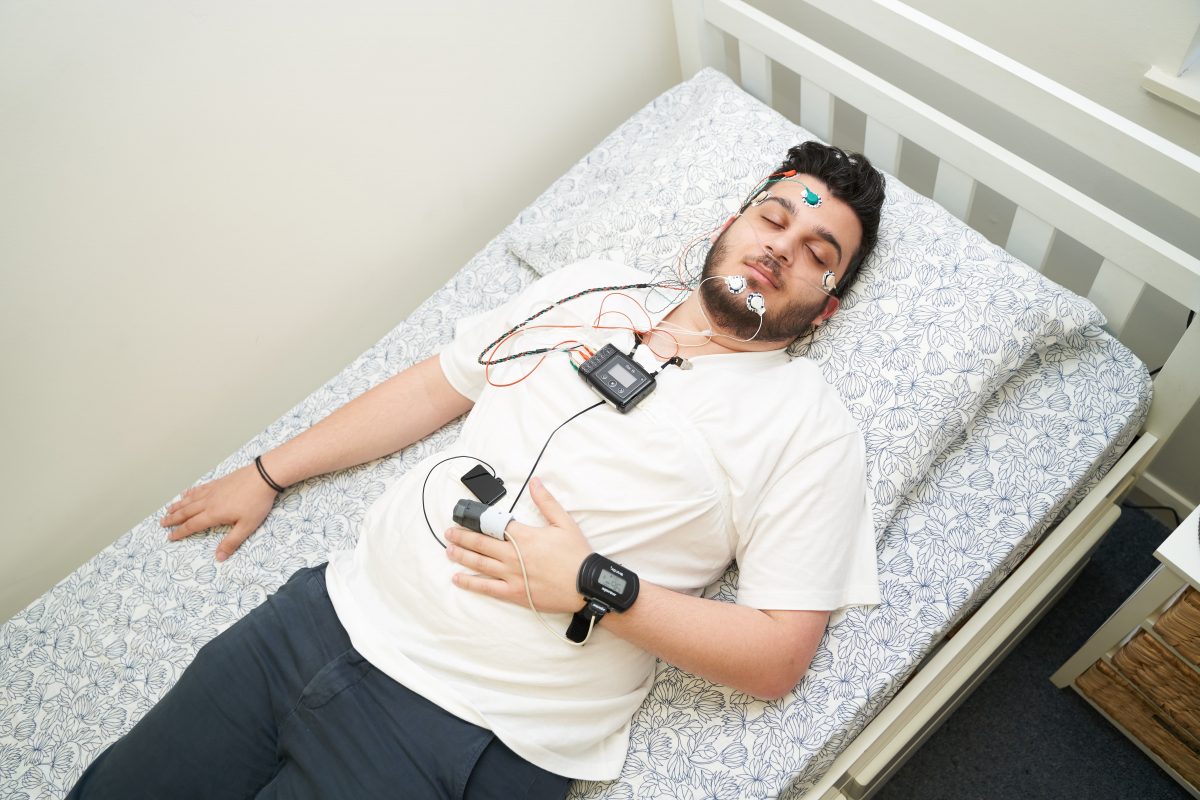
In most cases, they will wear a finger probe for oxygen, a nasal cannula for airflow, and a chest or abdomen belt for breathing effort. In the morning, the device is removed and returned for analysis.
Is a home sleep study accurate enough compared with a sleep lab?
For suspected obstructive sleep apnoea in adults, home sleep studies can be highly useful and clinically accepted. They are especially effective when the likelihood of moderate to severe OSA is high and symptoms are clear.
A sleep lab may still be preferred when the diagnosis is uncertain or when other conditions are suspected, such as complex insomnia, parasomnias, narcolepsy, or certain neurological or heart-related sleep issues. If the home test is negative but symptoms are strong, clinicians may recommend further testing.
What makes home testing more comfortable?
They can sleep in their own bed, follow their usual routine, and avoid the stress of an unfamiliar environment. For many people, that alone improves sleep quality on the test night.
Home testing can also feel less intrusive. While sensors are still worn, there are fewer wires than a full laboratory polysomnography, and there is no need to travel at night or arrange overnight supervision.
How do they prepare for a home sleep study night?
They should aim for a typical night so the results reflect normal sleep. That usually means following their usual bedtime and avoiding major schedule changes.
Clinics commonly advise limiting alcohol, avoiding naps late in the day, and keeping caffeine earlier than usual. They should also confirm with the provider whether regular medications should be taken as normal, as stopping medicines without guidance can be unsafe.
What do the results actually show, and what do they mean?
The report usually includes an index of breathing events per hour, oxygen saturation trends, and snoring or position effects if measured. This helps estimate severity and guide next steps.
If obstructive sleep apnoea is found, the results may be described as mild, moderate, or severe. Clinicians also look at oxygen lows and total time spent below certain oxygen thresholds, as that can influence urgency and treatment decisions.
What are the common next steps after a positive test?
If the test indicates sleep apnoea, they are usually offered a treatment plan based on severity, symptoms, and health risks. Many people are assessed for CPAP therapy, which keeps the airway open with gentle air pressure.
Other options may include a mandibular advancement splint fitted by a qualified dental sleep provider, positional therapy for back-sleeping apnoea, weight and lifestyle support, and management of nasal obstruction. Follow-up is important because comfort, mask fit, and adherence often determine success.

How do they choose a home sleep study provider in Sydney?
They should choose a provider that offers clear clinical oversight, not just a device drop-off. A good service explains what the test can and cannot diagnose, how results are interpreted, and what support is available after the report.
It also helps to check practical details: turnaround time, whether a GP referral is required, how the device is collected or posted, and whether a consultation with a sleep physician is included. Transparent pricing and access to treatment pathways are often signs of a well-run service. Check out more about the need of sleep study referral in Australia.
What should they do if the home test is “normal” but symptoms continue?
They should not ignore ongoing symptoms, because a single night of data may not capture every issue. Some people sleep differently on the test night, and some sleep disorders are not well assessed by home studies.
If tiredness, choking sensations, or loud snoring persist, clinicians may recommend repeating the study, switching to a laboratory study, or investigating other causes such as insomnia, restless legs, medication effects, depression, thyroid issues, or chronic nasal blockage.
How can they make the test night more successful?
They should set the device up earlier in the evening so there is no rush at bedtime. A quick check that sensors are secure can prevent data loss and the need to repeat the study.
It also helps to keep the bedroom environment normal: comfortable temperature, usual pillow setup, and minimal disruptions. If they wake in the night, they should avoid removing sensors unless instructed, then try to return to sleep as usual.
What is the simplest takeaway for people considering home sleep testing in Sydney?
A home sleep study in Sydney is often the fastest, most comfortable way to check for obstructive sleep apnoea. It can move them from “something feels off” to a clear plan, without the delay and hassle of a sleep lab.
If symptoms are affecting daytime functioning or health, a home test is a practical next step, especially when paired with proper clinical review and follow-up care.
FAQs (Frequently Asked Questions)
What is a home sleep study and what conditions does it test for?
A home sleep study is an overnight test conducted in the comfort of your own bed using a small, portable monitoring device. It primarily assesses breathing-related sleep disorders, especially obstructive sleep apnoea (OSA), by tracking airflow, oxygen levels, breathing effort, heart rate, and body position to estimate how often breathing reduces or stops during sleep.
Who in Sydney should consider undergoing a home sleep study?
Individuals experiencing symptoms such as loud snoring, witnessed pauses in breathing, gasping at night, morning headaches, or persistent daytime tiredness should consider a home sleep study. It is also recommended for people with high blood pressure, type 2 diabetes, atrial fibrillation, weight gain potentially linked to sleep apnoea, or those in safety-critical jobs involving driving or machinery operation.
How quickly can I get tested and receive results from a home sleep study in Sydney?
Many providers in Sydney can arrange home sleep testing within days or even within the same week depending on referrals and device availability. Results are typically available within a few business days after returning the device; however, timing may vary if specialist review or appointments are required.
How accurate is a home sleep study compared to an in-lab sleep study?
Home sleep studies are highly useful and clinically accepted for diagnosing suspected obstructive sleep apnoea in adults, particularly when symptoms indicate moderate to severe OSA. However, for uncertain diagnoses or other complex conditions like insomnia or narcolepsy, an in-lab polysomnography may be preferred. If the home test is negative but symptoms persist strongly, further testing might be recommended.
What should I expect during the home sleep study night?
You will be guided on how to apply sensors such as a finger probe for oxygen levels, a nasal cannula for airflow, and a chest or abdomen belt for breathing effort. The setup is designed to be simple so you can sleep as normally as possible while the device records data overnight. In the morning, you remove the device and return it for analysis.
What are the next steps if my home sleep study indicates obstructive sleep apnoea?
If obstructive sleep apnoea is diagnosed, your healthcare provider will offer a treatment plan based on severity and health risks. Common treatments include CPAP therapy to keep airways open with gentle air pressure. Other options may involve mandibular advancement splints from dental specialists, positional …