Chronic respiratory conditions like Chronic Obstructive Pulmonary Disease (COPD) and bronchiectasis present a significant health burden in Australia. Effective mucus clearance is often the “missing link” in maintaining lung function and preventing hospital admissions.
The Aerobika Oscillating Positive Expiratory Pressure (OPEP) device has emerged as a gold-standard, drug-free intervention. In this comprehensive 2026 guide, we explore the clinical evidence, including how it reduces COPD exacerbations by 28%, and provide a step-by-step framework for patients and clinicians to optimize airway clearance.
See more: Home Sleep Study Sydney: Fast and Comfortable Testing Options
What is the Aerobika OPEP Device?
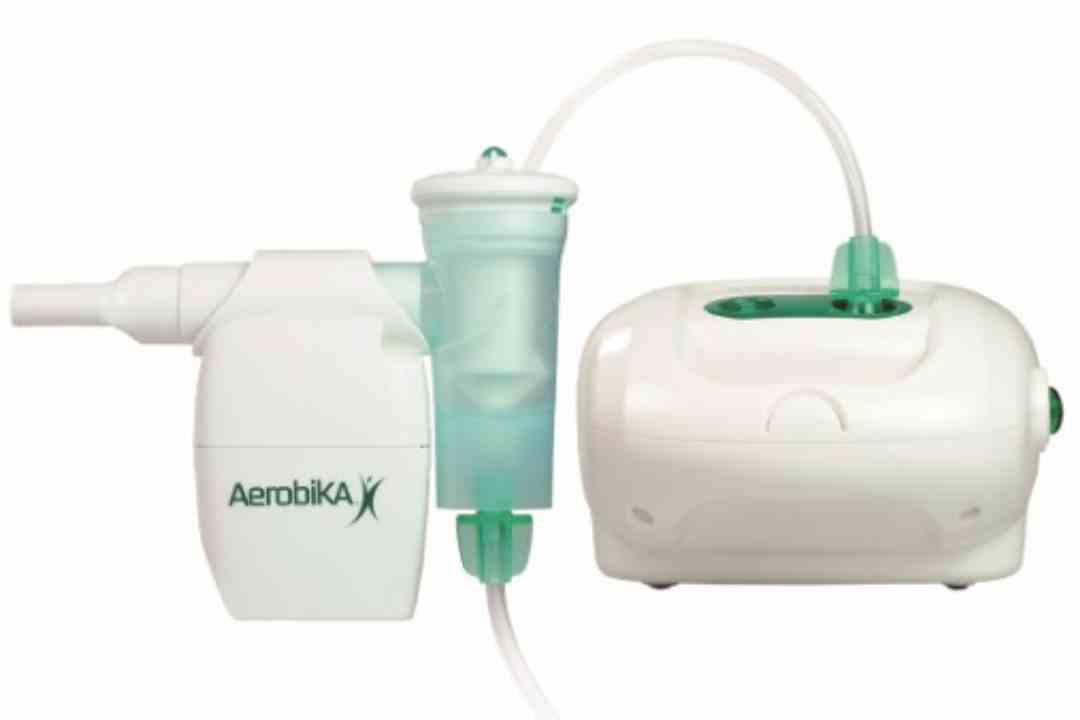
The Aerobika OPEP is a handheld, drug-free medical device designed to assist in the mechanical clearance of excess mucus from the lungs. It is particularly effective for patients with “wet” lung conditions where secretions obstruct the airways.
Unlike standard PEP devices, the Aerobika uses a unique pressure-oscillation mechanism. When you exhale into the device, it creates pulses of resistance (oscillations). These pulses serve two primary functions:
- Airway Stenting: The positive pressure keeps the smaller airways open, allowing air to get behind the mucus.
- Vibrational Shearing: The oscillations create high-frequency vibrations that thin and “shake” mucus free from the airway walls, moving it toward the larger airways where it can be coughed out easily.
Clinical Benefits: Why the Aerobika OPEP Ranks for COPD and Bronchiectasis
Clinical research has solidified the Aerobika OPEP’s role in modern respiratory management. In Australia, where COPD affects roughly 1 in 13 Australians aged 40 and over, these statistics are vital for long-term health outcomes.
1. 28% Reduction in COPD Exacerbations
A landmark real-world study demonstrated that using the Aerobika OPEP device reduces moderate-to-severe COPD flare-ups by 28% within 30 days of initial use following a hospital discharge. This is critical because 1 in 5 patients hospitalized for an exacerbation are often readmitted within a month.
2. Improved Lung Ventilation
Using hyperpolarized 3He MRI imaging, researchers have observed significant improvements in gas distribution throughout the lungs after 3–4 weeks of use. This suggests that the device doesn’t just clear mucus; it actively helps “re-open” areas of the lung that were previously under-ventilated.
3. Synergistic Effect with Nebulisers
The Aerobika is uniquely designed to be used simultaneously with certain nebulisers (like the AeroEclipse* BAN). This dual therapy allows medication to penetrate deeper into the opened airways, potentially increasing the efficacy of bronchodilators or saline treatments while reducing overall therapy time.
4. Enhanced Quality of Life
Patients reported significant improvements in:
- Exercise Tolerance: Increased distance in the 6-minute walk test (6MWD).
- Reduced Breathlessness: Lower scores on the St. George’s Respiratory Questionnaire (SGRQ).
- Symptom Control: Fewer paroxysmal coughing fits throughout the day.
How to Use the Aerobika OPEP: A Step-by-Step Process
Proper technique is essential for achieving the therapeutic goals of OPEP therapy. Follow this clinician-approved framework:
Step 1: Preparation and Setting
Ensure your hand does not block the exhalation path on the back of the device. Set the Resistance Indicator (a slider on the side) to the level prescribed by your physiotherapist. There are five settings; higher resistance provides more intense oscillations.
Step 2: Inhalation
- Sit upright with your shoulders relaxed.
- Take a deep breath in through your nose, slightly deeper than a normal breath.
- Hold your breath for 2 to 3 seconds. This allows the air to distribute evenly throughout the lungs (collateral ventilation).
Step 3: Active Exhalation
- Place the mouthpiece in your mouth and create a tight seal with your lips.
- Exhale actively but not forcefully.
- Your exhalation should last roughly 3 to 4 times longer than your inhalation.
- Keep your cheeks flat; you should feel the “vibrations” in your chest, not your face.
Step 4: The Cycle
Repeat for 10 to 20 breaths. After the cycle, perform 2–3 “huff coughs” (exhaling forcefully with an open mouth, like fogging up a mirror) to move the loosened mucus out of the throat.

Maintenance and Hygiene Standards
To prevent lung infections, specifically for patients with bronchiectasis or cystic fibrosis, strict cleaning is required.
| Frequency | Action | Method |
| After Each Use | Basic Wash | Disassemble into 4 parts. Wash in warm soapy water and air dry. |
| Daily | Disinfection | Top-rack dishwasher safe OR soak in 1:3 vinegar/water solution for 1 hour. |
| Weekly | Deep Sterilisation | Boil disassembled parts for 5 minutes (using a rack to avoid the hot base). |
Note: Replace the device every 12 months for optimal performance.
Common Mistakes and How to Avoid Them
- Blowing Too Hard: Excessive force can cause airway collapse. Aim for “active” rather than “forced” exhalation.
- Puffing the Cheeks: This absorbs the vibrations. Keep your cheeks firm to ensure the energy reaches your lungs.
- Ignoring the Resistance Setting: Starting too high can be fatiguing. Always consult a physiotherapist to find your optimal “sweet spot.”
- Skipping the Huff Cough: The device loosens the mucus, but the huff cough is the “vehicle” that removes it.
Internal Linking & References
Internal Linking Suggestions:
- Airway Clearance Techniques for Bronchiectasis
- Managing COPD Flare-ups in Winter
- The Role of Physiotherapy in Australian Respiratory Care
Authoritative External References:
- Lung Foundation Australia (COPD-X Guidelines)
- Thoracic Society of Australia and New Zealand (TSANZ)
FAQ: Frequently Asked Questions
What is the best resistance setting for Aerobika?
There is no “universal” setting. Your physiotherapist will determine the setting (1–5) based on your lung capacity and the viscosity of your mucus.
Can I use the Aerobika if I don’t have mucus?
While primarily for mucus clearance, the positive pressure can help with lung expansion in “dry” COPD cases, though its primary clinical benefit is for sputum producers.
Does the Aerobika require a prescription in Australia?
No, it is available over-the-counter and through respiratory specialists, but it is highly recommended to use it under the guidance of a healthcare professional.
How often should I use the device?
Typically, twice daily (morning and evening) is the standard. During a chest infection or exacerbation, your doctor may increase this to 4 times daily.
Is Aerobika better than the Flutter or Acapella?
The Aerobika is not position-dependent (it works while sitting, standing, or lying down) and has stronger clinical data regarding the reduction of hospital readmissions compared to older OPEP models.
Conclusion
The Aerobika OPEP device is a cornerstone of modern respiratory management in 2026. By reducing COPD exacerbations by 28% and providing a drug-free pathway to clearer lungs, it empowers patients to take control of their chronic conditions. Whether you are managing bronchiectasis or seeking to prevent the next COPD flare-up, the key to success lies in consistent use and proper technique.